Hemostatic Dressing: The Science and Application of Advanced Hemorrhage Control (2026)
In high-threat environments, the three minutes following a catastrophic hemorrhage are the most critical you will ever face. Selecting the wrong hemostatic dressing or failing to understand its chemical interaction with blood can result in treatment failure when margins are thinnest. You likely know that outdated concerns about exothermic reactions and chemical burns are no longer relevant with 2026 standards; yet, the choice between Kaolin-based and Chitosan-based agents remains a point of hesitation for many operators. It is a valid concern because gear is only as effective as the technician's confidence in it.
We will resolve that ambiguity by mastering the technical specifications, biological mechanisms, and tactical applications of modern hemostatics to stop life-threatening bleeding faster. You'll gain a clear understanding of clotting pathways and the ability to choose the right agent for your mission profile. This guide breaks down the CoTCCC-recommended protocols and refines your wound-packing technique to ensure field reliability when every second counts.
Key Takeaways
- Integrate advanced hemorrhage control into the MARCH algorithm to prioritize life-saving interventions under high-stress conditions.
- Evaluate the chemical mechanisms of Kaolin and Chitosan to select the optimal hemostatic dressing for your specific operational environment.
- Learn the "Power Pack" wound-packing technique to deliver sustained direct pressure to deep junctional hemorrhages.
- Secure your IFAK against failure by identifying CoTCCC-recommended hardware and avoiding the risks of counterfeit medical gear.
- Develop mission-ready proficiency by utilizing inert training aids to bridge the gap between clinical knowledge and tactical execution.
Understanding the Role of Hemostatic Dressings in Tactical Medicine
A hemostatic dressing is a specialized medical gauze treated with active agents designed to accelerate the body's natural clotting process. Unlike standard cotton gauze, which functions solely through mechanical absorption and pressure, these dressings utilize chemical or mucoadhesive properties to stop bleeding where traditional methods fail. In the high-stress environment of tactical medicine, every second dictates the outcome between survival and mortality. These tools are no longer optional extras; they are fundamental components of modern trauma kits.
The application of these dressings is a core requirement within the MARCH algorithm. This acronym prioritizes Massive Hemorrhage as the first critical intervention. While tourniquets handle extremity injuries, a hemostatic dressing is the primary solution for junctional wounds in the neck, axilla, or groin. Standard gauze often fails in these high-pressure environments because arterial flow can wash out a developing clot before it stabilizes. The chemical impregnated into the dressing ensures the clot adheres to the vessel wall, even under significant physiological pressure.
The Committee on Tactical Combat Casualty Care (CoTCCC) maintains rigorous standards for these interventions. Looking toward 2026, CoTCCC recommendations emphasize the use of dressings that are easy to pack, remain stable in extreme temperatures, and possess a high safety profile. Adhering to these evidence-based guidelines ensures that operators utilize the most effective technology available for life-saving interventions. The focus remains on products that have been rigorously tested in laboratory and field settings to ensure they perform under the duress of combat.
The Evolution of Hemorrhage Control
Tactical medicine has moved away from the early granular powders that once dominated the market. In the early 2000s, zeolite-based products were effective but produced significant heat. These exothermic reactions often caused secondary thermal burns to both the patient and the medic. This risk led to a shift toward impregnated gauzes that provide the same clotting speed without the heat. Modern QuikClot hemostatic dressings now use kaolin, a naturally occurring mineral that activates Factor XII in the clotting cascade without any exothermic side effects. The current gold standard for field hemostatics is a non-heat-generating, flexible gauze impregnated with kaolin or chitosan that initiates rapid coagulation through direct chemical interaction with blood components.
Preventable Death and the Golden Hour
Data from recent conflicts indicates that hemorrhage remains the leading cause of preventable death on the battlefield. Statistics show that roughly 90% of combat fatalities occur before the casualty reaches a definitive care facility. Out of those deaths, 80% are due to uncontrolled hemorrhage. Rapid intervention within the first 3 minutes of an arterial injury is the only way to prevent exsanguination. Hemostatic dressings play a vital role in extending the survivability window during the extraction phase. By securing the wound early, medics buy time for the "Golden Hour" of surgical intervention. Effective hemorrhage control includes several key advantages:
- Rapid Clot Formation: Achieving hemostasis in as little as 2 to 3 minutes of manual pressure.
- Stability: Maintaining clot integrity during patient transport over rugged terrain.
- Reduced Fluid Loss: Preserving blood volume to prevent the onset of lethal triad complications.
Stopping the bleed isn't just about the immediate moment. It's about ensuring the patient survives the long transit to a Level II or Level III medical facility. Without these advanced dressings, the risk of re-bleeding during movement increases by 45%, threatening the casualty's stability during the most vulnerable part of the evacuation. Using these tools correctly ensures the medic maintains control of the situation until higher-level care is available.
How Hemostatic Agents Accelerate the Clotting Cascade
Hemostasis isn't a single event. It's a complex, multi-stage biological chain reaction. When a major artery or vein is breached, the body initiates the clotting cascade to seal the leak. This process involves a sequence of chemical reactions where inactive proteins in the blood become active enzymes. Most modern hemostatic dressings target specific points in this sequence to force a clot faster than the body can manage alone. Understanding the mechanisms of hemostatic agents is vital for any operator managing a life-threatening hemorrhage in the field. These agents don't just soak up blood; they chemically alter the wound environment to create a stable, pressurized plug. By bypassing certain steps in the natural cascade, these tools reduce the time to achieve hemostasis from 10 minutes down to less than 180 seconds.
Kaolin: The Intrinsic Pathway Activator
Kaolin is a naturally occurring clay mineral. It acts as a potent catalyst for the body's intrinsic clotting pathway. When Kaolin contacts blood, it immediately triggers Factor XII, also known as the Hageman factor. This activation sets off a rapid-fire sequence of protein conversions that lead to the production of thrombin and, eventually, a dense fibrin net. This is the technology found in QuikClot Combat Gauze. The U.S. military adopted this specific hemostatic dressing as the primary standard of care in 2008 because it's stable and effective across extreme environments. The mineral is typically embedded into a non-woven gauze carrier. This carrier provides a mechanical framework that keeps the active agent in direct contact with the ruptured vessel wall. It allows the operator to pack the wound tightly, ensuring the chemical reaction happens exactly where the pressure is applied. This combination of chemical activation and physical packing is why Kaolin-based products remain a staple in IFAKs globally.
Chitosan: The Mucoadhesive Sealant
Chitosan is a biopolymer derived from the shells of crustaceans. It functions through a mechanism called mucoadhesion, which is fundamentally different from mineral-based agents. Chitosan molecules carry a strong positive charge. Since red blood cells carry a negative charge, the two bond instantly upon contact. This creates a sticky, gel-like seal over the injury site. The major tactical advantage of Chitosan is that it works independently of the body's natural clotting factors. It doesn't need the patient's enzymes to be functioning correctly to stop the bleed. This makes it a critical intervention for patients suffering from hypothermia or those who are on prescription blood thinners like Warfarin. In cold-weather operations where the body's natural enzymatic processes slow down, Chitosan remains effective. Products like Celox use this technology to create a robust clot even when the blood is too thin to coagulate on its own. This independence from the biological cascade ensures a higher probability of survival in complex trauma cases.
Safety is a primary concern when introducing foreign materials into a deep wound. Operators often ask about shellfish allergies regarding Chitosan. Clinical testing shows that the proteins responsible for shellfish allergies are removed during the manufacturing process, making the risk of an allergic reaction nearly zero. Systemic absorption is also not an issue; the agents stay localized to the wound bed. The goal is stability. A mucoadhesive hemostatic dressing prevents the clot from washing away if the patient's blood pressure spikes or during the rigors of tactical evacuation. This level of reliability is why you should always train with high-quality medical gear to ensure your skills match the capability of your equipment. Effective hemorrhage control requires both the right chemistry and the right technique. By using these agents, you're not just covering a wound; you've engineered a structural solution to a lethal problem.
Kaolin vs. Chitosan: Evaluating Modern Hemostatic Technologies
Selecting the right hemostatic dressing requires an objective analysis of chemical efficacy and logistical constraints. Kaolin based products, such as Combat Gauze, utilize a naturally occurring mineral to trigger the intrinsic clotting pathway. This mechanism accelerates the body's natural ability to form a stable clot. Chitosan based agents, like Celox or ChitoGauze, operate through a different process. These are mucoadhesive polysaccharides derived from shellfish. They carry a positive charge that attracts negatively charged red blood cells, creating a physical "plug" independent of the body's clotting cascade. This makes Chitosan particularly effective for patients in coagulopathy or those using blood thinners.
Logistical factors often dictate procurement for large agencies. Both technologies typically offer a 5 year shelf life when stored in original vacuum sealed packaging. Storage requirements are similar; both remain stable in temperatures ranging from -30°F to 140°F. However, Chitosan can become brittle if the packaging is compromised in high humidity environments. Agencies must weigh the $45 to $55 per unit cost against the tactical necessity. While Kaolin remains a staple due to its widespread adoption, Chitosan’s ability to function regardless of the patient's physiological state provides a distinct advantage in trauma cases involving massive blood loss.
Packaging design is a critical factor in rapid deployment. Z-fold configurations have largely replaced traditional rolled gauze in professional kits. A Z-fold allows the operator to feed the gauze directly into the wound track without the risk of the roll dropping and unravelling in the dirt. This configuration saves approximately 15 to 20 seconds during the initial packing phase. Every professional hemostatic dressing should include a radiopaque marker. This strip is visible under X-ray, ensuring surgeons can identify and remove all foreign material during definitive care in the operating room.
Performance in Adverse Environments
Temperature extremes rarely degrade the chemical integrity of these agents, but they do affect the handling of the carrier gauze. In wet or rainy conditions, Chitosan based dressings often outperform Kaolin. The mucoadhesive properties of Chitosan create a tacky gel when exposed to fluid, which helps the material adhere to the wound walls during high pressure arterial spurting. According to the TCCC Guidelines for Hemostatic Dressings, both agents are highly effective, but the physical bond formed by Chitosan provides a slight edge in "washout" scenarios where blood volume is significant.
Mission-Specific Selection Criteria
Law enforcement officers operating in urban environments prioritize speed and kit profile. Short evacuation times to Level 1 trauma centers mean a compact 3 inch by 4 yard Z-fold gauze is often sufficient for their IFAK. Wilderness medics or those in prolonged field care roles may opt for larger Chitosan dressings. These offer better protection against re-bleeding during the extended transport times common in remote operations. For the universal operator kit, MED-TAC recommends a 3 inch by 4 yard Z-fold Kaolin or Chitosan gauze. It's the industry standard for a reason. It fits in low-visibility kits and provides the necessary surface area to pack most junctional wounds effectively.
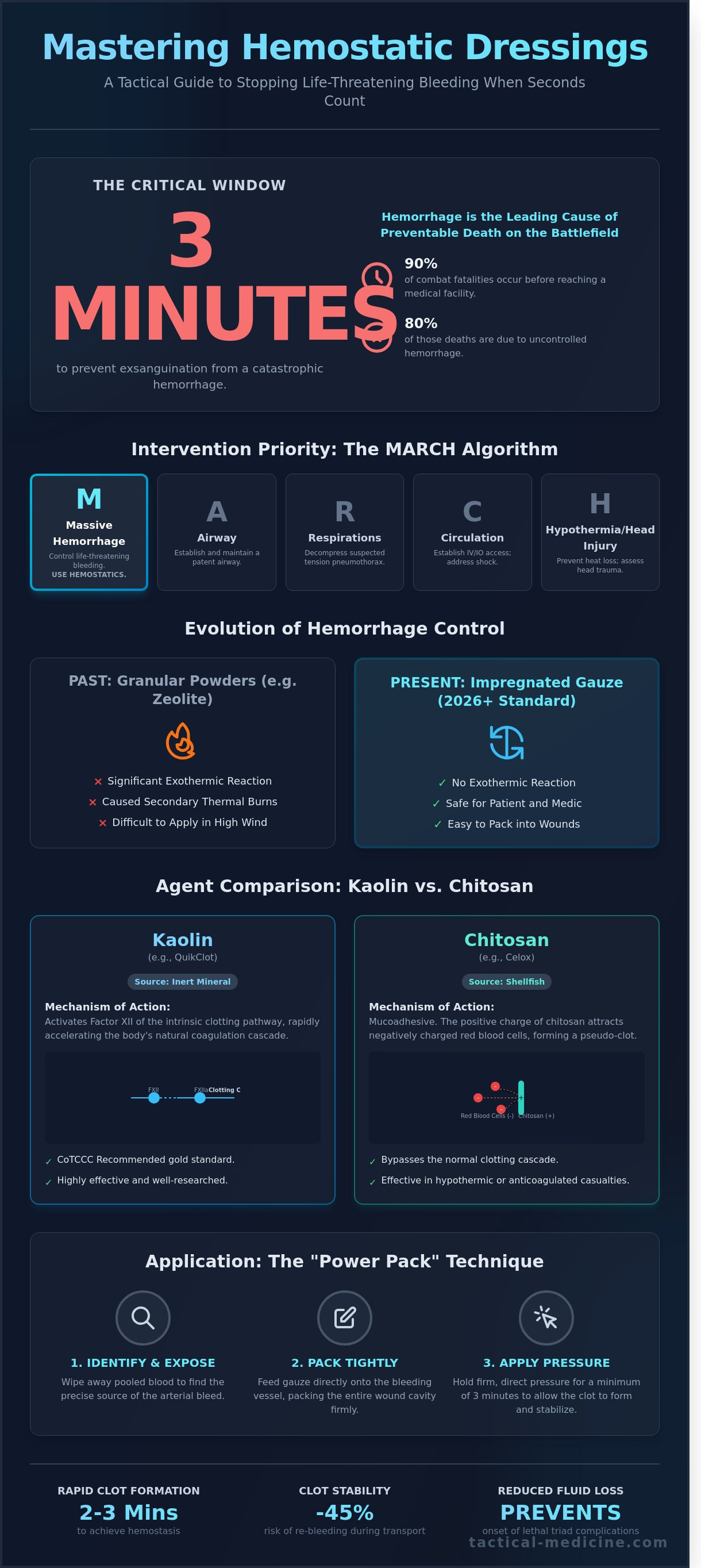
Step-by-Step Wound Packing with Hemostatic Gauze
A hemostatic dressing isn't a passive medical supply. It's a tool that requires aggressive, manual intervention to function correctly. The chemical agents impregnated in the gauze, whether kaolin or chitosan, rely on intimate contact with the bleeding vessel to initiate the clotting cascade. If you simply place the gauze on top of a wound, it'll fail. You must apply direct, focused pressure to the "leak" to achieve physiological control. In tactical environments, this means using your weight to compress the artery against the bone.
The "Power Pack" technique is the gold standard for deep junctional wounds in the groin or axilla. You must identify the specific point of hemorrhage before you begin. Once the source is located, you'll feed the gauze into the cavity, ensuring every cubic centimeter of space is occupied. This creates a mechanical plug while the chemical agent works. You're not just filling a hole; you're building a structural dam against arterial pressure.
The Mechanics of Effective Wound Packing
Success depends on the finger-over-finger technique. Start by creating a "pilot ball" of gauze and pushing it directly onto the bleeding vessel. Never lose contact with that point. Use one finger to hold the gauze in place while the other hand feeds more material in. This maintains constant pressure on the source. You've used enough material when the wound is packed tightly and the gauze is slightly mounded above the skin level. This ensures that when you apply a secondary wrap, the pressure is transmitted downward into the wound track.
Once the cavity is packed, transition to a pressure dressing like the Israeli Bandage or an H-Bandage. These devices maintain the tension you've created manually. Ensure the plastic pressure bar is positioned directly over the wound site to maximize downward force. According to CoTCCC 2024 guidelines, the transition from manual pressure to a mechanical bandage must be deliberate to avoid shifting the internal pack.
Post-Packing Protocols
Packing the wound is only half the battle. You must maintain manual pressure for at least 180 seconds immediately after the cavity is filled. This 3-minute window allows the hemostatic agents to react with the blood and form a stable clot. Don't peek. If you release pressure too early to check your work, you risk dislodging the initial fibrin mesh and restarting the hemorrhage. If the dressing becomes saturated with bright red, pulsing blood during this time, your pack has failed. You must remove the old material and start over with a fresh hemostatic dressing to find the true source of the leak.
- Monitor for Re-bleeding: Check the site every 5 to 10 minutes, especially during patient movement or transport.
- Documentation: Use a permanent marker to record the time of application and the specific agent used on the TCCC card.
- Securing the Tail: Ensure any excess gauze is tucked under the pressure wrap so it doesn't snag during extraction.
In high-stress scenarios, your fine motor skills will degrade. Practice these steps until the finger-over-finger motion is muscle memory. The goal is a dense, hard pack that stops the flow entirely. Clinical data from battlefield interventions shows that effective packing can achieve a 90% success rate in controlling junctional hemorrhage when these specific protocols are followed. Your discipline during these three minutes determines the patient's survival during the evacuation phase.
Selecting Battle-Proven Hemostatic Gear for Your IFAK
Don't gamble with third-party marketplaces when your life is on the line. Unverified sellers often distribute medical gear that hasn't undergone any clinical testing or quality control. A 2019 report from the Committee on Tactical Combat Casualty Care (CoTCCC) warned that counterfeit medical supplies are increasingly prevalent on global platforms. These fakes look identical to genuine products but lack the essential kaolin or chitosan impregnation required to stop a massive hemorrhage. In a high-threat environment, you have approximately 180 seconds to intervene before exsanguination becomes a certainty. Using a substandard hemostatic dressing during those 3 minutes is a fatal mistake. We source every product directly from manufacturers to eliminate the risk of "gray market" inventory.
The integrity of your Individual First Aid Kit (IFAK) depends on the authenticity of its components. Counterfeit gauze often fails when the operator applies the 50-80 psi of pressure required for effective wound packing. Genuine agents are designed to withstand these physical demands while simultaneously initiating the clotting cascade. We maintain a strict chain of custody for all tactical medical hardware to ensure that the gear you carry is the gear that works. Reliability isn't a luxury; it's a mission requirement.
Combat-Ready vs. Training-Grade Materials
Opening your mission-ready gear for practice is a critical failure. Once the vacuum seal breaks, moisture degrades the active chemical agents and compromises sterility. Use inert trainers to bridge the gap between theory and application. High-fidelity simulators provide the tactile feedback needed to master wound packing under stress without wasting life-saving components. Refine these skills by enrolling in MED-TAC Training Courses for professional, hands-on certification.
The MED-TAC Standard for Hemorrhage Control
Our selection follows the evidence-based protocols established by the CoTCCC. We prioritize QuikClot Combat Gauze and Celox Rapid due to their 90% success rate in field trials and combat deployments. Our veteran-owned model ensures every item integrates perfectly into the MARCH algorithm. We vet every National Stock Number (NSN) to guarantee authenticity and performance in extreme environments. Equip your team with CoTCCC-recommended hemostatic dressings today.
Before you deploy your kit into the field, you must conduct a thorough audit of your bleeding control supplies. Medical gear is not a "set it and forget it" asset. Environmental factors like heat and friction can damage packaging over time, especially if the kit is worn on a plate carrier or belt. Use the following checklist to ensure your hemostatic dressing is ready for immediate intervention:
- Inspect the vacuum seal: If the packaging feels loose or contains air, the seal is compromised and the product must be replaced.
- Verify expiration dates: Most hemostatic agents have a 5-year shelf life. Replace any items within 6 months of their "Use By" date.
- Confirm CoTCCC approval: Look for the specific branding of QuikClot, Celox, or ChitoGauze to ensure you aren't carrying a generic substitute.
- Accessibility check: Ensure your dressing is positioned for one-handed access. You shouldn't be digging through loose items to find your primary hemostatic agent.
- Training currency: Review your training logs. If you haven't performed a full-speed wound packing drill in the last 180 days, your muscle memory is likely degrading.
Maintaining your gear is as important as the initial purchase. A professional operator treats their medical kit with the same discipline as their primary weapon system. By sourcing battle-proven materials and committing to regular training, you ensure that you're prepared to provide effective care under fire. Success in tactical medicine is the result of deliberate preparation and the refusal to accept substandard equipment.
Secure the Advantage in Critical Hemorrhage Control
Effective hemorrhage control isn't a matter of chance; it's a discipline rooted in evidence-based protocols. The evolution of hemostatic dressing technology since its 2004 tactical debut has shifted the survival curve for non-compressible junctional wounds. You've analyzed how Chitosan-based agents and Kaolin-impregnated gauze like QuikClot Combat Gauze provide distinct physiological advantages during the clotting cascade. Adhering to the MARCH algorithm requires more than just owning gear. It demands a 3-minute commitment to manual pressure and precise wound packing techniques that bridge the gap between injury and surgery. Data from 2024 field reports indicates that proper application reduces mortality rates by 30% in massive extremity trauma.
We provide the exact tools used by Tier 1 units globally. As a 100% veteran-founded and operated team, we ensure every item in our inventory meets current CoTCCC compliance standards. We're a professional TCCC and TECC certification provider dedicated to your operational readiness. Equip your IFAK with field-proven hardware that doesn't fail when the mission is on the line. Your skill is the weapon; let our gear be your edge.
Shop Professional-Grade Hemostatic Dressings
Train hard and stay prepared for the next intervention.
Frequently Asked Questions
Do hemostatic dressings cause burns like they used to?
Modern hemostatic dressing options don't cause burns. Original zeolite granules released in 2002 produced exothermic reactions reaching 150 degrees Fahrenheit, but current CoTCCC recommended products like QuikClot Combat Gauze utilize kaolin. This mineral initiates the clotting cascade without generating heat. You can apply these dressings to open wounds without risking thermal injury to the casualty or the provider.
Can I use hemostatic gauze on someone with a shellfish allergy?
You can safely use chitosan based gauze on patients with shellfish allergies. While chitosan's derived from shrimp shells, the manufacturing process removes the proteins responsible for allergic triggers. Testing conducted in 2011 showed zero adverse reactions among 10 subjects with confirmed hypersensitivity. Always follow the MARCH algorithm and prioritize hemorrhage control over theoretical allergy concerns in life threatening scenarios.
How long can a hemostatic dressing be left in a wound?
You should leave a hemostatic dressing in place for no more than 24 hours. These materials are designed for temporary hemorrhage control during the tactical evacuation phase. Clinical protocols dictate that surgical teams must remove the packing in a sterile environment to prevent infection or vascular complications. Ensure you document the exact time of application on the TCCC casualty card to inform higher levels of care.
Is hemostatic gauze better than a tourniquet?
Neither tool is superior; their application depends entirely on the wound location. Use a CoTCCC recommended tourniquet for life threatening bleeds on limbs where a cuff can be placed 2 to 3 inches above the injury. Use gauze for junctional wounds in the groin, neck, or armpit where a tourniquet cannot reach. Effective wound packing requires 3 minutes of direct pressure to ensure the agent reacts with the blood.
What is the difference between QuikClot and Celox?
The primary difference lies in their chemical mechanism for achieving hemostasis. QuikClot utilizes kaolin, a mineral that activates Factor XII in the body's natural clotting cascade. Celox uses chitosan, a mucoadhesive that bonds with red blood cells to form a gel like plug. Because Celox doesn't rely on the body's internal clotting factors, it remains effective even when the casualty is hypothermic or in coagulopathy.
Can I reuse a hemostatic dressing for training?
You must never reuse a hemostatic dressing for training or clinical use. These products are vacuum sealed and sterilized for single use applications. Once the seal's broken, the material's subject to environmental degradation and bacterial contamination. Use dedicated training gauze, which lacks the active hemostatic agent, to practice your packing techniques on high fidelity manikins. This preserves your life saving stock for real world interventions.
Does hemostatic gauze work on patients taking blood thinners?
Hemostatic gauze is effective on patients using anticoagulant medications like Coumadin or Eliquis. Chitosan based products are particularly useful because they create a physical seal through cross linking with red blood cell membranes. This process bypasses the chemical clotting cascade that blood thinners inhibit. In 2015, clinical trials confirmed that these dressings successfully controlled hemorrhage in patients with compromised coagulation profiles.
Where should I store hemostatic dressings in my IFAK?
Store your dressings in the primary, rip away section of your IFAK for immediate access. Massive hemorrhage is the first priority in the MARCH algorithm and can cause death within 120 seconds. You shouldn't be digging through secondary pouches to find your packing material. Ensure the expiration date's visible through the packaging and check the vacuum seal for integrity every 30 days during gear inspection.



Leave a comment